Blood tests are an essential part of understanding your overall health, and the Complete Blood Count (CBC) is one of the most common tests doctors order.
Among the many components of a CBC, MCH, or Mean Corpuscular Hemoglobin, is a key measurement that helps evaluate the health of your red blood cells.
Simply put, MCH indicates the average amount of hemoglobin present in each red blood cell, which is vital for carrying oxygen throughout your body. Abnormal MCH levels can signal underlying health issues such as anemia, vitamin deficiencies, or other blood disorders.
Understanding what MCH means, its normal range, and the implications of low or high levels can help you make sense of your blood test results and guide you toward appropriate medical care.
In this article, we’ll explore everything you need to know about MCH in blood tests, including causes, symptoms, and ways to maintain healthy levels.
What Is MCH in a Blood Test?
MCH, or Mean Corpuscular Hemoglobin, is an important measurement in a Complete Blood Count (CBC) test. It tells doctors how much hemoglobin, the oxygen-carrying protein, is present in each red blood cell. Hemoglobin is critical because it transports oxygen from the lungs to tissues and organs, supporting energy production and overall body function.
The MCH value is calculated by dividing the total hemoglobin by the number of red blood cells in a blood sample. The result is expressed in picograms (pg) per cell, giving an average amount of hemoglobin per red blood cell. While it does not indicate the total hemoglobin in your blood, MCH helps physicians understand the quality and function of your red blood cells.
MCH is closely related to other red blood cell indices like MCV (Mean Corpuscular Volume), which measures the size of red blood cells, and MCHC (Mean Corpuscular Hemoglobin Concentration), which measures the concentration of hemoglobin in a red blood cell. By evaluating these values together, doctors can identify different types of anemia and other blood disorders more accurately.
Abnormal MCH levels may indicate various health conditions. Low MCH often points to iron deficiency anemia, while high MCH could signal vitamin B12 or folate deficiency. Regular monitoring of MCH, especially as part of a CBC test, can provide crucial insights into your overall blood health and guide appropriate treatment.
What Does MCH Stand For?
MCH stands for Mean Corpuscular Hemoglobin, which essentially means the average amount of hemoglobin contained in each red blood cell. Breaking it down: “Mean” refers to the average, “Corpuscular” refers to the individual red blood cell (or corpuscle), and “Hemoglobin” is the protein that carries oxygen. Together, it provides a snapshot of how much oxygen-carrying protein each red blood cell holds.
Understanding what MCH stands for is important because it gives context to your blood test results. While hemoglobin levels alone tell you the total amount in your blood, MCH focuses on individual cells. For example, two people could have the same total hemoglobin levels, but if one has very small red blood cells, the MCH will be lower, indicating potential anemia.
The MCH value is calculated using a simple formula:MCH (pg)=RBC count (millions/µL)Hemoglobin (g/dL)×10
This calculation gives an average amount of hemoglobin per red blood cell in picograms (pg). A normal MCH usually ranges between 27–33 pg in adults, but slight variations can occur depending on the lab and the individual’s age or gender.
Knowing what MCH stands for also helps when interpreting related values, like MCV and MCHC, which together paint a clearer picture of red blood cell health. Abnormalities in MCH may indicate low hemoglobin content (hypochromia) or high hemoglobin content (macrocytosis), signaling possible deficiencies or underlying medical conditions.
Normal MCH Range
The normal MCH range is an important benchmark in understanding your red blood cell health. MCH measures the average amount of hemoglobin in each red blood cell, and doctors use it alongside other indices to evaluate conditions like anemia or vitamin deficiencies.
For most adults, the typical MCH range is 27–33 picograms (pg) per cell. Slight variations may exist depending on the laboratory or testing equipment used. Children may have slightly different ranges, and in some cases, reference ranges are adjusted for age and gender. Knowing your personal reference range is essential, as even minor deviations can provide early clues about potential health issues.
A normal MCH value indicates that your red blood cells contain a healthy amount of hemoglobin, allowing them to efficiently carry oxygen throughout the body. When MCH falls within the normal range, it usually suggests that your red blood cells are functioning well, your iron and vitamin levels are sufficient, and there are no obvious blood-related disorders.
However, a normal MCH does not always rule out problems. For example, someone could have a normal MCH but still experience anemia if other red blood cell indices, such as MCV or MCHC, are abnormal. Therefore, doctors typically evaluate MCH together with the complete blood count (CBC) to get a full picture of your blood health.
Understanding the normal MCH range empowers you to interpret your blood test results more effectively and discuss them confidently with your healthcare provider.
What Does Low MCH Mean?
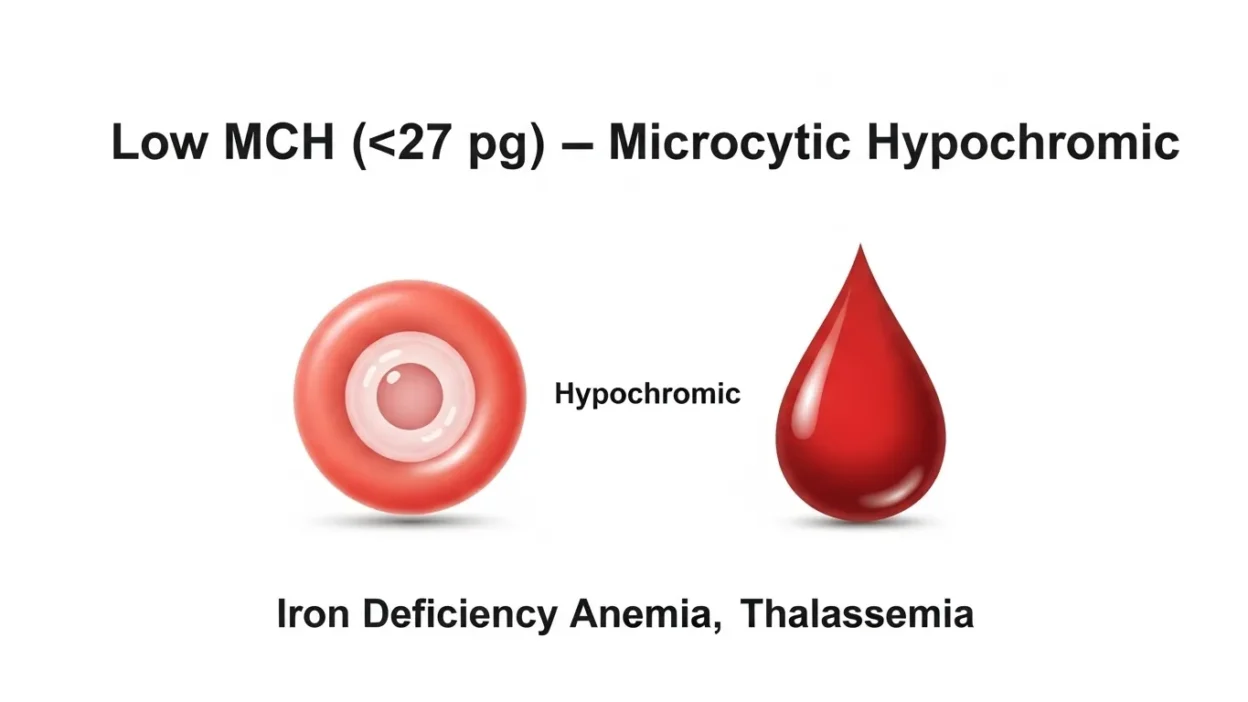
A low MCH means that each of your red blood cells contains less hemoglobin than normal. Since hemoglobin is responsible for carrying oxygen to tissues and organs, low MCH can affect your body’s ability to deliver sufficient oxygen, leading to fatigue, weakness, and other symptoms. In medical terms, low MCH is often referred to as hypochromic red blood cells, which literally means “less color,” because hemoglobin gives red blood cells their characteristic red hue.
Low MCH is usually detected as part of a Complete Blood Count (CBC) test. Doctors don’t rely on MCH alone—they also consider related indices such as MCV (red blood cell size) and MCHC (hemoglobin concentration) to understand the type of anemia or blood disorder a patient might have.
Common symptoms associated with low MCH include:
- Fatigue and general weakness
- Pale or sallow skin
- Shortness of breath during physical activity
- Dizziness or lightheadedness
- Rapid heartbeat
It’s important to note that low MCH itself is not a disease, but rather a sign of an underlying condition. Most often, it points to forms of anemia, particularly iron deficiency anemia, but it may also result from chronic diseases, blood loss, or nutritional deficiencies. Early detection of low MCH allows healthcare providers to identify and treat these conditions before they lead to more serious complications.
Monitoring MCH levels regularly, along with other CBC components, can provide valuable insight into your overall blood health and guide effective treatment strategies.
Causes of Low MCH
Low MCH usually indicates that red blood cells contain less hemoglobin than normal, and this can occur due to several underlying causes. Understanding these causes helps doctors identify the specific type of anemia or health condition affecting your blood.
1. Iron Deficiency Anemia
The most common cause of low MCH is iron deficiency. Iron is essential for producing hemoglobin, and a lack of it can lead to smaller, less efficient red blood cells. Causes of iron deficiency include poor dietary intake, blood loss from heavy periods, gastrointestinal bleeding, or chronic conditions that affect iron absorption.
2. Thalassemia
Thalassemia is a genetic disorder that affects hemoglobin production. People with this condition often have low MCH, smaller red blood cells, and chronic anemia. It is inherited and typically identified through specialized blood tests.
3. Chronic Diseases
Certain chronic illnesses, such as kidney disease, infections, or inflammatory disorders, can reduce hemoglobin production, resulting in low MCH. This is sometimes referred to as anemia of chronic disease.
4. Nutritional Deficiencies
Deficiencies in essential nutrients like vitamin B6, folate, or copper can also lower MCH. While iron is the most common culprit, these other nutrients are critical for proper red blood cell formation.
5. Blood Loss
Significant blood loss, whether from injury, surgery, or gastrointestinal bleeding, can lower hemoglobin levels and subsequently reduce MCH.
Low MCH is often a signal rather than a diagnosis. Identifying the exact cause is crucial for effective treatment. Doctors may recommend iron supplements, dietary changes, or further testing depending on the underlying condition.
What Does High MCH Mean?
A high MCH indicates that each of your red blood cells contains more hemoglobin than normal. While this might sound beneficial, it can actually signal underlying health issues that affect red blood cell production or size. High MCH is often associated with macrocytic red blood cells, meaning the cells are larger than normal and contain more hemoglobin per cell.
High MCH is usually discovered during a Complete Blood Count (CBC) test, and doctors consider it alongside other red blood cell indices such as MCV (Mean Corpuscular Volume) and MCHC (Mean Corpuscular Hemoglobin Concentration). Evaluating these together helps determine the type and cause of anemia or other blood disorders.
Common symptoms that may accompany high MCH include:
- Fatigue or weakness
- Pale or yellowish skin
- Shortness of breath
- Memory or concentration problems
- Dizziness
High MCH itself is not a disease but a marker indicating a possible deficiency or disorder. The most common causes include vitamin B12 or folate deficiency, which affects red blood cell maturation, and certain liver or thyroid conditions that impact blood cell formation. Alcohol consumption and some medications can also contribute to elevated MCH levels.
Recognizing a high MCH early allows healthcare providers to investigate underlying causes and recommend appropriate treatment, such as vitamin supplementation, lifestyle changes, or managing chronic health conditions. Regular blood tests help monitor MCH and ensure red blood cells are functioning optimally.
Causes of High MCH
A high MCH means that your red blood cells carry more hemoglobin than normal, which often reflects larger-than-average red blood cells, known as macrocytes. Understanding the causes of high MCH helps doctors identify potential nutritional deficiencies, chronic conditions, or lifestyle factors affecting blood health.
1. Vitamin B12 Deficiency
Vitamin B12 is essential for proper red blood cell production. A deficiency can lead to the production of larger red blood cells with more hemoglobin, resulting in high MCH. Symptoms of B12 deficiency may include fatigue, tingling in hands and feet, and memory problems.
2. Folate Deficiency
Folate (vitamin B9) works closely with B12 in red blood cell development. A lack of folate can cause macrocytic anemia, raising MCH levels. Common causes include poor diet, pregnancy, or certain medications that affect folate metabolism.
3. Liver Disease
Chronic liver conditions can affect the production and lifespan of red blood cells. This may lead to abnormally large red blood cells, increasing MCH. Elevated MCH in this context often appears alongside other abnormal liver-related blood markers.
4. Hypothyroidism
An underactive thyroid can slow metabolism and disrupt red blood cell formation. This can result in macrocytosis and higher MCH levels, sometimes accompanied by fatigue, weight gain, and cold intolerance.
5. Alcohol Use
Excessive alcohol consumption affects bone marrow and red blood cell production, leading to larger, immature cells with higher hemoglobin content, increasing MCH.
High MCH is usually a warning sign rather than a disease itself. Identifying the underlying cause—whether nutritional, medical, or lifestyle-related—is essential for proper treatment. Doctors may recommend supplements, dietary changes, or management of chronic conditions to normalize MCH levels.
Difference Between MCH, MCV, and MCHC
When reviewing blood test results, you may notice MCH, MCV, and MCHC. While all three are red blood cell indices, they measure different aspects of red blood cells and help doctors diagnose anemia or other blood disorders.
1. MCH (Mean Corpuscular Hemoglobin)
MCH measures the average amount of hemoglobin per red blood cell. Hemoglobin is the protein responsible for carrying oxygen. Low MCH indicates less hemoglobin per cell (hypochromia), while high MCH indicates more hemoglobin per cell (macrocytosis).
2. MCV (Mean Corpuscular Volume)
MCV measures the average size of red blood cells. Small red blood cells (microcytic) often correlate with low MCH, while large red blood cells (macrocytic) usually correlate with high MCH. MCV is critical for classifying anemia types.
3. MCHC (Mean Corpuscular Hemoglobin Concentration)
MCHC measures the concentration of hemoglobin in a red blood cell rather than the total amount. It helps identify whether red blood cells are pale (hypochromic) or overly saturated with hemoglobin (hyperchromic).
How Doctors Use Them Together
Doctors rarely interpret MCH, MCV, or MCHC in isolation. For example:
- Low MCH + Low MCV → Iron deficiency anemia
- High MCH + High MCV → Vitamin B12 or folate deficiency
- Normal MCH + Abnormal MCV → Other types of anemia or chronic disease
By comparing these three values, healthcare providers get a complete picture of red blood cell health, allowing for accurate diagnosis and targeted treatment. Understanding the difference between MCH, MCV, and MCHC empowers patients to make sense of their blood test results and engage in informed discussions with their doctors.
How Doctors Interpret MCH Results
When doctors review MCH results from a Complete Blood Count (CBC) test, they consider the value in the context of other red blood cell indices, overall hemoglobin levels, and the patient’s health history. MCH alone does not provide a complete picture but is a key piece of the puzzle in evaluating blood health.
Evaluating MCH With MCV and MCHC
- Low MCH + Low MCV: This combination typically suggests iron deficiency anemia or conditions causing smaller-than-normal red blood cells (microcytosis).
- High MCH + High MCV: Indicates macrocytic anemia, often caused by vitamin B12 or folate deficiency, liver disease, or hypothyroidism.
- Normal MCH with abnormal MCV or MCHC: Can point to other blood disorders or chronic illnesses that may not directly affect hemoglobin content per cell but impact red blood cell size or concentration.
Symptoms and Patient History
Doctors also consider clinical symptoms such as fatigue, pale skin, or shortness of breath, along with dietary habits, medication use, and underlying conditions. For example, patients with chronic kidney disease may have normal MCH but still suffer from anemia due to low erythropoietin levels.
Follow-Up Testing
Abnormal MCH results often prompt additional blood tests, including iron studies, vitamin B12 and folate levels, or reticulocyte counts, to pinpoint the cause. This approach ensures accurate diagnosis and effective treatment.
In summary, MCH is a valuable indicator of red blood cell health, but doctors always interpret it alongside other blood parameters. By looking at patterns rather than isolated values, healthcare providers can identify specific types of anemia, nutritional deficiencies, or other blood-related disorders and provide tailored medical guidance.
How to Improve Low MCH Levels
Low MCH indicates that each red blood cell carries less hemoglobin than normal, often due to iron deficiency or other nutritional shortages. Improving MCH levels usually involves addressing the underlying cause through diet, supplements, and lifestyle changes.
1. Iron-Rich Diet
Since iron is essential for hemoglobin production, consuming iron-rich foods can help raise MCH levels. Examples include:
- Red meat, liver, and poultry
- Spinach, kale, and other leafy greens
- Lentils, beans, and chickpeas
- Fortified cereals and whole grains
Pairing iron-rich foods with vitamin C sources like oranges, tomatoes, or bell peppers enhances iron absorption.
2. Iron Supplements
For significant deficiencies, doctors may recommend oral iron supplements. These should always be taken under medical supervision, as excessive iron can cause side effects like stomach upset or constipation.
3. Address Underlying Health Conditions
Low MCH may also result from chronic illnesses such as kidney disease or blood loss. Treating these conditions, whether through medication, surgery, or other interventions, can help normalize MCH levels over time.
4. Balanced Nutrition
In addition to iron, vitamins B6, B12, and folate are essential for healthy red blood cell production. Including eggs, dairy, fortified cereals, and leafy vegetables supports overall hemoglobin synthesis.
5. Regular Monitoring
Regular CBC tests allow your doctor to track MCH levels and ensure treatments are effective. Gradual improvements are normal, and lifestyle changes combined with medical guidance are the safest way to restore healthy red blood cell function.
By following these steps, individuals with low MCH can improve oxygen transport in the blood, boost energy levels, and support overall health.
How to Reduce High MCH Levels
A high MCH indicates that each red blood cell contains more hemoglobin than normal, often due to larger-than-average red blood cells (macrocytosis). While MCH itself is not a disease, elevated levels can signal nutritional deficiencies, chronic health conditions, or lifestyle factors. Reducing high MCH focuses on addressing the root cause.
1. Correct Vitamin Deficiencies
Vitamin B12 and folate deficiencies are the most common causes of high MCH. Increasing intake of these nutrients through diet or supplements can help normalize red blood cell size and hemoglobin content. Foods rich in B12 include eggs, dairy products, fish, and lean meats. Folate can be obtained from leafy greens, beans, and fortified cereals.
2. Manage Liver and Thyroid Health
Liver disease and hypothyroidism can contribute to high MCH. Treating underlying conditions, such as controlling thyroid hormone levels or managing liver function, often improves MCH levels over time.
3. Limit Alcohol Consumption
Excessive alcohol intake can interfere with red blood cell production, leading to macrocytosis and high MCH. Reducing or eliminating alcohol consumption can support healthy blood cell formation.
4. Regular Monitoring
Doctors may recommend follow-up blood tests to track MCH and related red blood cell indices. Monitoring ensures that interventions like diet changes or medical treatment are effectively normalizing blood parameters.
5. Medication Review
Certain medications, including chemotherapy drugs or anti-seizure medications, can increase MCH. Consulting with your healthcare provider about alternatives or dosage adjustments may be necessary.
By targeting the underlying cause, whether nutritional, medical, or lifestyle-related, high MCH levels can often be normalized, improving red blood cell health and overall oxygen delivery throughout the body.
When Should You Be Concerned About MCH Levels?
MCH levels provide important insight into the health of your red blood cells, but abnormal values don’t always indicate an immediate problem. Understanding when to be concerned helps you take timely action and prevent complications.
Signs to Watch For
If you experience fatigue, weakness, dizziness, shortness of breath, or pale skin, these symptoms could indicate that your red blood cells are not carrying enough oxygen. Even mild changes in MCH, when accompanied by these symptoms, warrant further investigation.
Abnormal Blood Test Results
Doctors usually become concerned when MCH is consistently outside the normal range (27–33 picograms in adults). Low MCH often points to iron deficiency anemia, while high MCH may indicate vitamin B12 or folate deficiency, liver disease, or hypothyroidism. In both cases, follow-up tests are essential to determine the underlying cause.
When to Seek Medical Attention
- Persistently low or high MCH levels
- Accompanying symptoms such as extreme fatigue, dizziness, or rapid heartbeat
- Underlying health conditions that may worsen with anemia or macrocytosis, like heart disease or chronic kidney disease
Importance of Professional Guidance
MCH abnormalities should never be ignored, even if you feel well. A doctor may recommend additional blood tests, nutritional assessments, or treatment plans to address the root cause. Early detection allows for targeted interventions, such as dietary changes, supplements, or medical management, which can restore healthy red blood cell function and prevent complications.
By monitoring MCH and consulting a healthcare provider when necessary, you can ensure that your blood remains healthy and capable of efficiently delivering oxygen throughout the body.
Related Blood Tests Doctors May Order
When doctors notice abnormal MCH levels, they often recommend additional blood tests to determine the underlying cause. These tests provide a more complete picture of red blood cell health and help identify specific deficiencies or disorders.
1. Hemoglobin Test
A hemoglobin test measures the total amount of hemoglobin in the blood. Since MCH represents the hemoglobin content per cell, comparing it with total hemoglobin helps doctors understand whether red blood cells are functioning properly.
2. Hematocrit Test
Hematocrit indicates the percentage of blood volume made up of red blood cells. Low hematocrit combined with low MCH may confirm iron deficiency anemia, while high hematocrit could point to other conditions like dehydration or polycythemia.
3. Reticulocyte Count
Reticulocytes are immature red blood cells. Measuring their count helps doctors evaluate bone marrow activity. Low reticulocyte levels can indicate decreased red blood cell production, while high levels may suggest the body is compensating for blood loss or hemolysis.
4. Iron Studies
Iron studies include serum iron, ferritin, and total iron-binding capacity (TIBC). These tests help identify iron deficiency, the most common cause of low MCH, and guide appropriate supplementation or treatment.
5. Vitamin B12 and Folate Tests
If MCH is high, doctors may check vitamin B12 and folate levels to rule out deficiencies that cause macrocytic anemia. Supplementing these vitamins often normalizes MCH and improves red blood cell health.
By ordering these related tests, healthcare providers can accurately diagnose the cause of abnormal MCH and create a tailored treatment plan. This comprehensive approach ensures that any blood or nutritional disorder is addressed effectively.
FAQs:
1. What is a good MCH level?
A healthy MCH level for most adults ranges from 27 to 33 picograms (pg) per red blood cell. Values within this range typically indicate that your red blood cells have a normal amount of hemoglobin and are functioning efficiently.
2. Is low MCH dangerous?
Low MCH itself is not a disease but a sign of an underlying condition, such as iron deficiency anemia. If left untreated, low MCH can lead to symptoms like fatigue, pale skin, dizziness, and shortness of breath. Early detection and treatment are important to prevent complications.
3. Is high MCH harmful?
High MCH may indicate macrocytic anemia caused by vitamin B12 or folate deficiency, liver disease, hypothyroidism, or certain medications. While not immediately dangerous, it signals that red blood cells are not forming properly, and the underlying cause should be addressed.
4. Can diet affect MCH levels?
Yes. Iron-rich foods, vitamin B12, folate, and a balanced diet can influence MCH levels. Iron deficiency often causes low MCH, while vitamin deficiencies may lead to high MCH. Proper nutrition supports healthy red blood cell production.
5. How often should MCH be checked?
MCH is part of a Complete Blood Count (CBC), which doctors may order annually or more frequently if you have symptoms or a history of anemia or other blood disorders. Regular monitoring helps track improvements or detect issues early.
Understanding MCH and its implications empowers patients to interpret their blood test results, take preventive steps, and seek medical guidance when needed.
Conclusion:
Understanding MCH (Mean Corpuscular Hemoglobin) is essential for interpreting your blood test results and maintaining healthy red blood cell function.
MCH measures the average amount of hemoglobin in each red blood cell, which is critical for transporting oxygen throughout your body.
Abnormal MCH levels either low or high can indicate underlying health issues such as iron deficiency, vitamin B12 or folate deficiency, chronic diseases, or liver and thyroid problems.
A low MCH often points to iron deficiency anemia, resulting in smaller red blood cells with less hemoglobin. Symptoms may include fatigue, pale skin, dizziness, and shortness of breath.
On the other hand, a high MCH indicates larger red blood cells with more hemoglobin, usually caused by macrocytic anemia, vitamin deficiencies, or chronic conditions.
Monitoring MCH levels is most effective when combined with other red blood cell indices such as MCV and MCHC, along with a thorough evaluation of your medical history and symptoms.
Addressing the underlying cause is key, whether it involves dietary improvements, supplementation, managing chronic conditions, or lifestyle changes like reducing alcohol intake.
Regular CBC blood tests allow healthcare providers to track MCH and related values over time, ensuring early detection and proper management of any blood-related issues.
By understanding what MCH means and taking proactive steps, you can maintain optimal red blood cell health, improve oxygen delivery in the body, and support overall well-being.
Being informed about MCH empowers you to have meaningful discussions with your doctor, interpret your blood test results confidently, and take timely action to maintain your health.

Welcome to TextFlirtz.com, your ultimate destination for fun, flirty, and clever pick-up lines that spark conversations and make hearts skip a beat! Whether you’re looking to impress your crush, add some humor to your chats, or just have a playful time texting, we’ve got you covered with lines that are witty, spicy, and unforgettable. Dive in, explore our collections, and start flirting the smart way—because at TextFlirtz.com, words are your best wingman!